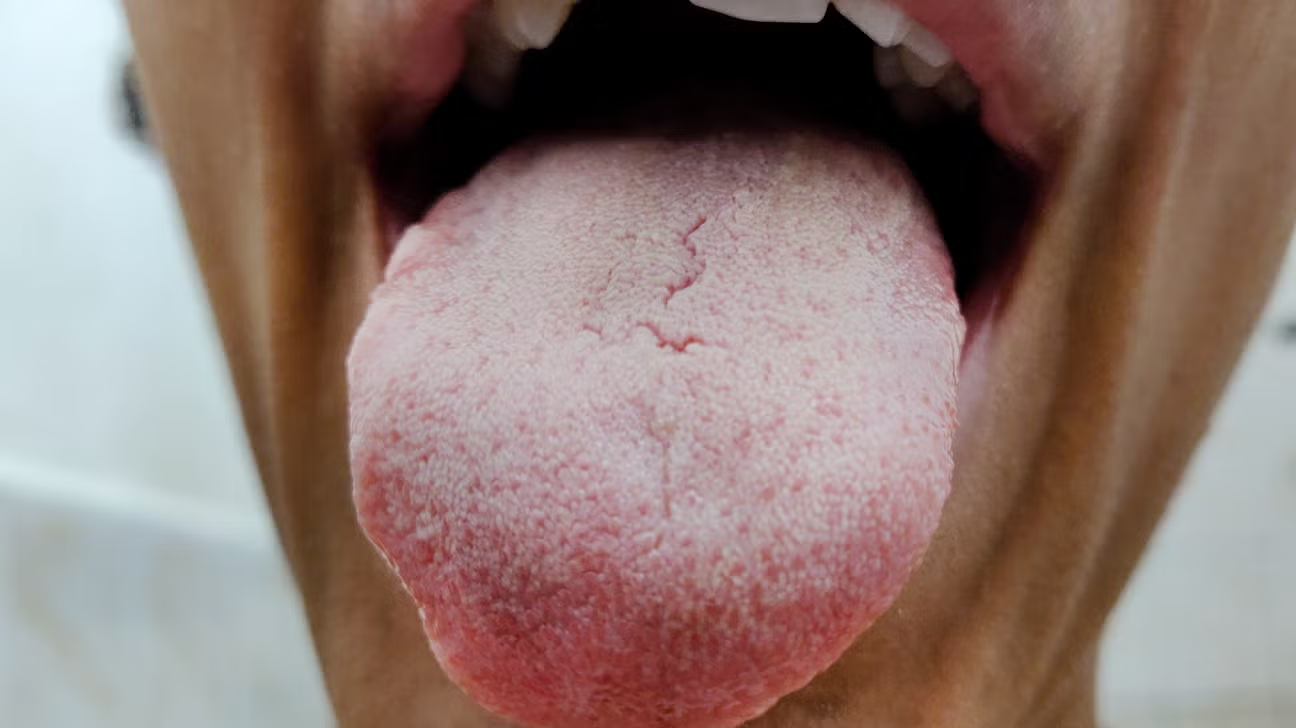
You wake up in the morning, shuffle to the bathroom, and catch a glimpse of your tongue in the mirror. Something looks off. There is a thick, whitish film sitting on the surface — almost like a light layer of frost covering the tongue from back to front. You brush your teeth, rinse, and hope it disappears. Sometimes it does. Sometimes it does not.
If this sounds familiar, you are not alone. A coated tongue is one of the most common oral health complaints that adults experience at some point in their lives. Most people brush it off — no pun intended — as nothing more than a morning annoyance. But what many do not realize is that the appearance of your tongue can serve as a surprisingly accurate window into what is happening inside your body.
The coating you see is not random. It is made up of bacteria, dead skin cells, food particles, and various debris that have become trapped between the tiny projections on the surface of your tongue. When these pile up, they create that milky or chalky layer that changes the color and texture of the tongue entirely.
The good news is that in most cases, a coated tongue is harmless and easy to deal with at home. But in certain situations, it is your body’s way of flagging something that deserves attention. This article covers everything — the causes, what different coatings mean, how to treat it, when to see a doctor, and how to prevent it from coming back. By the time you are done reading, you will know exactly what your tongue is trying to tell you.
What Exactly Is a Coated Tongue?
The Science Behind It — What Is Happening on Your Tongue’s Surface
Your tongue is covered with thousands of tiny raised projections called papillae. These papillae play a key role in taste and help with the early stages of digestion. Under normal circumstances, they sit flat, stay clean through saliva production, and do not cause any visible coating.
The problem begins when these papillae become swollen or elongated. As they grow in size, the gaps between them widen, and that creates the perfect environment for debris to get trapped. Bacteria, dead epithelial cells, food remnants, and even yeast organisms settle in and build up over time. The result is a visible, often unpleasant coating that sits on the surface of the tongue.
It is important to understand that a coated tongue is not a disease in itself. It is a symptom — a visible sign produced by one or more underlying causes. The coating can vary in thickness, texture, and color depending on what is driving it. A thin, slightly white coating that clears up after your morning glass of water is generally considered normal. A thick, persistent, or unusually colored coating is not.
This distinction matters a great deal, and it is why understanding the causes is the essential first step before jumping to any kind of treatment.
Common Causes of a Coated Tongue
There is rarely just one reason why someone develops a coated tongue. Most of the time, it is a combination of daily habits, dietary choices, and in some cases, an underlying health condition. Here are the most well-established causes, broken down clearly.
Poor Oral Hygiene
This is the number one reason most adults develop a coated tongue. When you do not brush your tongue regularly — or skip flossing — bacteria and dead cells accumulate rapidly on the surface. The longer they sit, the thicker the coating becomes. Many people brush their teeth twice a day without ever touching their tongue. That leaves the back portion of the tongue, which is the most prone to buildup, completely neglected.
Using a tongue scraper or the back of a soft-bristled toothbrush to clean the tongue as part of your daily routine can make an enormous difference in just a few days.
Dehydration and Dry Mouth
Saliva is your mouth’s natural cleaning agent. It washes away bacteria, neutralizes acids, and keeps the surface of your tongue moist and clean. When your body is dehydrated or when saliva production drops for any reason, the natural cleansing process slows down significantly. Debris builds up faster, and the tongue begins to develop that characteristic coating.
Dry mouth, or xerostomia, is also a common side effect of many prescription medications — including antihistamines, antidepressants, and blood pressure medications. If you have noticed your tongue looking worse since starting a new medication, this may be why.
Diet and Lifestyle Habits
What you eat and drink plays a bigger role than most people expect. Diets that are high in sugar, refined carbohydrates, dairy, and alcohol create the exact conditions that bacteria and yeast thrive in. These foods essentially feed the organisms responsible for the coating.
Smoking and tobacco use are also major contributors. Tobacco introduces toxic compounds into the oral environment that irritate tongue tissue directly. Over time, this irritation causes the papillae to become enlarged, making it easier for debris to collect and harder to clean away. Smokers are consistently more likely to develop a heavy coated tongue than non-smokers.
Oral Thrush — A Fungal Cause That Is Often Missed
Oral thrush is caused by an overgrowth of Candida — a type of yeast that lives naturally in the mouth in small amounts. When something disrupts the balance of your oral microbiome, Candida can multiply rapidly and cause a distinct white coating that looks almost like cottage cheese spread across the tongue and inner cheeks.
Oral thrush is more common in certain groups: newborns, elderly individuals, people with diabetes, and those with weakened immune systems. It is also frequently triggered by the use of steroid inhalers for asthma, or by a course of antibiotics that wipes out the good bacteria keeping yeast in check.
Unlike a standard coated tongue, oral thrush patches often cannot be scraped away easily, and they may cause a burning or sore sensation underneath.
Medications and Antibiotics
Antibiotics are incredibly effective at fighting bacterial infections — but they are non-selective. They eliminate harmful bacteria and beneficial bacteria alike. When the healthy bacteria in your mouth are wiped out by a course of antibiotics, the microbial balance shifts, and opportunistic organisms like Candida take over.
Beyond antibiotics, steroids, chemotherapy drugs, immunosuppressants, and certain inhalers have all been documented as causes of tongue coating. If you have recently completed a course of medication and noticed your tongue looking different, that is likely not a coincidence.
Underlying Health Conditions
In some cases, a persistent coated tongue points toward something systemic. Gastroesophageal reflux disease (GERD) can introduce stomach acid into the mouth repeatedly, altering the oral environment. Diabetes affects immune response and oral microbial balance. Autoimmune conditions like lichen planus can cause distinctive white patches on the tongue that are sometimes mistaken for a simple coating.
Leukoplakia — a condition characterized by thick white patches on the tongue or inside of the mouth — is another condition worth knowing about, as certain forms carry a risk of becoming cancerous over time. This is why any white patch that cannot be scraped off or that persists for more than two to three weeks should be evaluated by a professional.
What Does Tongue Color Tell You? Reading the White Coating on Your Tongue
One of the most practical skills you can develop when it comes to oral health is learning to read what the color and thickness of your tongue’s coating actually means. Not all coatings are the same, and each has its own implications.
Thin White Coating — Typically Normal
A thin, slightly moist whitish layer on the tongue’s surface in the morning is considered completely normal in healthy individuals. It forms overnight when saliva production slows and bacteria multiply in the absence of food or drink. This kind of coating is of no concern — it clears up with water and brushing.
Thick White or Milky Coating
A heavy, opaque coating that does not clear up after oral hygiene routine suggests something more. This is where bacterial overgrowth, oral thrush, or chronic dehydration are the most likely explanations. The coating may come with noticeably bad breath and a dulled or altered sense of taste.
Yellow Coating
A yellow coating is usually the result of accelerated buildup of dead skin cells combined with bacterial activity. It can also point toward poor digestion or, in more pronounced cases, liver stress. Improving oral hygiene typically resolves mild yellow coating within a week or two.
Brown or Black Hairy Tongue
This is rare and visually startling, but it is worth knowing about. Black hairy tongue occurs when the papillae on the tongue become dramatically elongated and stained by chromogenic bacteria. The tongue can look almost furry and dark. Heavy tobacco use, excessive coffee consumption, and prolonged antibiotic use are the most common causes. Despite looking severe, it often resolves with improved hygiene and lifestyle changes.
White Patches — Not the Same as a Coating
This distinction is critical. A white coating covers the tongue broadly and can usually be partially scraped away. White patches, on the other hand, are localized, may be raised or textured, and often cannot be removed by scraping. These may indicate leukoplakia or oral lichen planus, both of which require professional evaluation. Leukoplakia patches in particular can progress to oral cancer in a small percentage of cases, which is why they should never be ignored.
Symptoms That Often Accompany a Coated Tongue
A coated tongue rarely appears in isolation. It tends to come with a set of companion symptoms that can help you understand what is going on.
Bad breath (halitosis) is by far the most consistent accompanying symptom. The same bacteria responsible for the coating are the primary producers of volatile sulfur compounds — the compounds that cause unpleasant odors in the mouth.
Altered taste is another common complaint. People describe it as a metallic, bitter, or muted sensation. The coating acts almost like a physical barrier between taste buds and food, making flavors seem less sharp.
A dry or furry sensation on the tongue is typically linked to dehydration or medication-induced dry mouth.
Soreness or a burning feeling are signs to take more seriously. These suggest the coating may be related to oral thrush, lichen planus, or another condition that involves actual tissue irritation rather than simple buildup.
If your coated tongue comes with no pain, clears up with brushing, and is a consistent light white, home care is almost certainly sufficient. If pain, patches, or persistence are part of the picture, it is time to look further.
How to Treat a Coated Tongue at Home
For the vast majority of people, a coated tongue is entirely manageable at home with a few consistent habits. Here is what actually works.
Daily Habits That Make a Real Difference
Tongue scraping is the single most effective tool for removing buildup. A good-quality tongue scraper — used with gentle back-to-front strokes each morning — removes the debris layer far more efficiently than brushing alone. Rinse the scraper after each pass and follow with water.
Brushing technique matters. Use a soft-bristled toothbrush twice daily. After cleaning your teeth, extend the brush to your tongue and clean the surface using gentle back-to-front strokes. Focus especially on the back of the tongue, which is where the heaviest buildup tends to occur.
Stay hydrated. Drinking at least eight glasses of water a day keeps saliva production consistent and helps wash away debris naturally throughout the day.
Use an antibacterial mouthwash after scraping and brushing for an added layer of protection. Mouthwash used on its own without prior scraping has limited effect — the physical removal comes first.
Adjust your diet. Cutting back on sugar, alcohol, and dairy can reduce the food supply available to bacteria and yeast. Adding raw crunchy vegetables like carrots and celery to your meals creates a natural mechanical cleaning effect as you chew.
Quit or reduce tobacco use. This single change can dramatically improve the appearance and health of the tongue within weeks. The irritation caused by tobacco is one of the hardest factors to overcome with hygiene alone.
What to Expect and How Long It Takes
For a standard coated tongue caused by hygiene or dehydration, consistent home care typically shows visible results within three to five days. A full resolution usually takes no more than one to two weeks. If the coating remains after two weeks of diligent effort, or if it is heavily discolored, that is your cue to seek professional advice.
When You Need Professional Treatment for a Coated Tongue
Home care is excellent for the everyday variety of coated tongue, but there are clear situations where professional input is not optional.
Signs It Is Time to See a Dentist or Doctor
You should book an appointment if any of the following apply:
- The coating has persisted for more than two to three weeks despite consistent oral hygiene.
- You have white patches on the tongue that cannot be scraped off.
- The coating is accompanied by pain, a burning sensation, or difficulty swallowing.
- The coating is yellow, brown, or black.
- You have recently been on a long course of antibiotics or steroids.
- You have a health condition such as diabetes or a compromised immune system.
Medical Treatments Depending on the Cause
The treatment a doctor or dentist recommends will depend entirely on what is causing the coated tongue in your specific case.
Oral thrush is treated with antifungal medications. These come in several forms — a topical gel or lozenge for mild cases, or an oral antifungal pill for more persistent infections. Nystatin and fluconazole are the most commonly prescribed options.
Bacterial overgrowth in certain cases may require a targeted antibiotic, though improving oral hygiene is often the primary intervention.
Leukoplakia is monitored carefully by a dental professional. If there is a risk of malignancy, removal via laser therapy, scalpel excision, or cryotherapy may be recommended.
Oral lichen planus is typically managed with corticosteroid treatments to reduce inflammation, combined with regular monitoring over time.
The underlying message here is that persistent or unusual presentation of a coated tongue should never be self-diagnosed and self-treated indefinitely. A professional can differentiate between the harmless and the serious quickly and accurately.
Coated Tongue in Special Populations
While anyone can develop a coated tongue, certain groups face a higher risk and may require additional attention.
Newborns and infants are particularly prone to oral thrush. New parents sometimes mistake the white coating of oral thrush for residual milk — the key difference is that milk residue wipes away cleanly, while thrush does not. A pediatrician can confirm the diagnosis and prescribe a safe antifungal treatment.
Elderly individuals experience naturally reduced saliva production as they age, and many take multiple medications that further dry out the mouth. This combination makes them significantly more susceptible to tongue coating, bacterial growth, and oral thrush.
People with diabetes present with distinctly heavier and more widespread tongue coating compared to the general population. Research shows that diabetic patients often exhibit thicker coating, larger affected surface areas, and a bluish discoloration of the tongue tissue — findings that highlight the direct relationship between systemic health and oral appearance.
Those undergoing chemotherapy or living with HIV have compromised immune systems, making them particularly vulnerable to Candida overgrowth and other oral infections that present as a coated tongue.
Preventing a Coated Tongue Long-Term
Prevention is always easier than treatment. Once you have cleared up a coated tongue, keeping it clear comes down to maintaining a consistent routine.
Building a Mouth-Care Routine That Actually Sticks
A genuinely effective oral hygiene routine for preventing a coated tongue includes: brushing twice daily with fluoride toothpaste, flossing or using interdental brushes every evening, tongue scraping every morning as a non-negotiable step, using an antiseptic mouthwash after brushing, and drinking adequate water throughout the day.
Scheduling a professional dental cleaning every six months ensures that any early signs of concern are caught and addressed before they become a bigger problem.
The Gut-Oral Connection Worth Knowing
There is a growing body of evidence pointing toward the relationship between gut health and oral health. Chronic acid reflux introduces stomach acid into the mouth repeatedly, altering the oral environment and making tongue coating more likely. Imbalances in the gut microbiome can also influence the composition of bacteria in the mouth.
Eating a diet rich in fiber, fermented foods, and diverse vegetables supports a healthier microbiome throughout the body — including the mouth. Some research suggests that probiotic supplementation may help restore oral microbial balance following antibiotic use, though this is an emerging area that continues to be studied.
Conclusion
A coated tongue is one of those health signals that most people notice but few people take seriously until it becomes persistent or uncomfortable. The truth is that your tongue’s appearance is a genuinely useful health indicator — one that can tell you a great deal about your oral hygiene habits, your diet, your hydration, and in some cases, your overall health.
In the majority of situations, a coated tongue responds quickly and completely to improved daily habits. Tongue scraping, better hydration, reducing sugar and tobacco, and keeping up with dental appointments are the building blocks of a clean, healthy tongue.
But the color, thickness, and persistence of your coating all carry meaning. A thin white morning film is normal. A thick, stubborn, or painful coated tongue that hangs around beyond two weeks is telling you something different. That is when home care is not enough, and a dentist or doctor becomes the right next step.
The white coating on your tongue does not have to be a mystery. Once you understand what causes it, what to look for, and how to respond, you are equipped to handle it confidently — and to know exactly when to ask for help.
FAQ 1: What is a coated tongue and what causes it?
A coated tongue is a visible white, yellowish, or grayish film that develops on the surface of the tongue when bacteria, dead skin cells, food debris, and sometimes yeast accumulate between the tiny papillae. It is not a standalone condition but a symptom produced by many potential causes Google Support, including poor oral hygiene, dehydration, smoking, medication use, and underlying health conditions such as oral thrush or GERD.
FAQ 2: Is a coated tongue a sign of a serious illness?
In most cases, a coated tongue is not a sign of serious illness. It is usually linked to oral hygiene or lifestyle factors rather than being a direct symptom of disease. Internetmarketingninjas However, if the coating is thick, discolored, painful, or lasts beyond two to three weeks despite good oral hygiene, it can indicate conditions such as oral thrush, leukoplakia, or a systemic issue that requires professional evaluation.
FAQ 3: How do I get rid of a coated tongue fast?
The fastest and most effective approach at home is consistent tongue scraping combined with proper brushing and good hydration. The best and easiest way to remove the coating from your tongue is with a tongue scraper. The practice involves scraping the tongue from back to front several times using light pressure, proceeding systematically from one side to the next, and rinsing your mouth with water or mouthwash afterward. SEOptimer Most harmless coatings clear up visibly within three to five days of this routine.
FAQ 4: Can a coated tongue go away on its own?
Yes, a mild coated tongue caused by dehydration, sleeping with your mouth open, or minor hygiene lapses will often resolve on its own. A harmless coating on the tongue, consisting of food debris, bacteria and dead cells, usually disappears with proper oral hygiene. Rankability However, a coating that does not clear up after two weeks or appears in an unusual color needs a doctor’s assessment rather than waiting it out.
FAQ 5: What does the color of tongue coating mean?
Tongue coating color is a practical health signal. A thin white coating is generally normal and clears with brushing. A thick white or milky coating points toward bacterial overgrowth or oral thrush. A yellow coating often suggests digestive imbalance or a fungal infection. Bacteria that normally live on the tongue produce pigments that are harmless but can cause the tongue to look brown, yellow, black, or even greenish. Quora A black or brown appearance, known as black hairy tongue, is rare and typically linked to tobacco, antibiotics, or excessive coffee use.
FAQ 6: Does a coated tongue cause bad breath?
Yes, bad breath is the most frequent accompanying symptom of a coated tongue, caused by gas-producing bacteria Internetmarketingninjas that thrive within the debris layer. These bacteria release volatile sulfur compounds, which are the primary source of unpleasant oral odors. Cleaning the tongue directly — through scraping and brushing — is the most effective way to reduce this odor at its source.
FAQ 7: Can medications cause a coated tongue?
Absolutely. A coating often develops following a course of antibiotics, which kill off the healthy bacteria in the mouth and allow yeast and other organisms to overgrow. Rankability Beyond antibiotics, steroids, asthma inhalers, antidepressants, antihistamines, and immunosuppressants are all documented causes of tongue coating. If you have noticed your tongue changing since starting a new medication, that connection is likely worth discussing with your prescribing doctor.
FAQ 8: What is the difference between a coated tongue and oral thrush?
Both conditions can create a white appearance on the tongue, but they are distinct. A standard coated tongue forms from accumulated debris, bacteria, and dead cells — and can usually be partially removed by scraping. A white tongue involves having a thick white film coating the tongue Sarah Worboyes, whereas oral thrush, caused by Candida overgrowth, creates white patches that resemble cottage cheese, often cannot be easily scraped away, and may leave a red or sore surface underneath when disturbed. Oral thrush requires antifungal treatment, while a standard coated tongue typically responds to improved hygiene.
FAQ 9: Can a coated tongue be a sign of diabetes?
Yes, research confirms a clear connection. The appearance of a coated tongue should be monitored among patients with diabetes, as yellow tongue coating has been associated with higher prevalence of diabetes mellitus and is linked with pre-diabetes. Cleveland Clinic Diabetic patients tend to produce less saliva, have altered immune responses, and face a higher risk of Candida overgrowth, all of which contribute to tongue coating. A yellow or unusually thick coating in a person with diabetes warrants discussion with their healthcare provider.
FAQ 10: Can a coated tongue occur during pregnancy?
Yes, pregnancy is a common time for tongue coating to worsen. Changing hormone levels during pregnancy can reduce saliva production, resulting in dry mouth, which leads to increased bacterial growth in the oral cavity and consequently a thicker coating on the tongue. Furthermore, during pregnancy, women need to be drinking for two and thus regularly become dehydrated Colgate, which further accelerates buildup. Pregnant women experiencing persistent coating should speak with their dentist or midwife, particularly since some treatments like antifungals require medical clearance during pregnancy.
FAQ 11: Does fasting cause a coated tongue?
Yes, fasting is a well-recognized trigger. When fasting, only liquid food is consumed, meaning the coating is not mechanically removed from the tongue by chewing, causing the tongue to remain coated. Using a tongue scraper as part of a fasting routine is a good idea. Rankability The reduced mechanical action of chewing solid food, combined with lower saliva flow during long fasting periods, creates the ideal conditions for tongue coating to accumulate and thicken.
FAQ 12: Can a coated tongue be a symptom of COVID-19?
There is evidence suggesting a connection. A recent study evaluating COVID-19-positive patients found that 25% of those diagnosed had mucocutaneous lesions in the oral cavity, with 50% of those lesions affecting the tongue. Typical presentation includes a whitish coating over the tongue alongside loss of taste, burning, ulceration, and white or red patches. Colgate The proposed mechanism involves the virus binding to oral epithelial cells and allowing opportunistic infections to take hold due to the compromised immune environment.
FAQ 13: Is a coated tongue linked to gut health or digestive problems?
There is a growing body of evidence supporting the gut-oral health connection. Conditions like gastroesophageal reflux disease (GERD) repeatedly introduce stomach acid into the oral cavity, disrupting the normal bacterial environment and encouraging coating. Similarly, imbalances in the gut microbiome can influence the bacterial composition of the mouth. Conditions like geographic tongue, lichen planus, glossitis, and systemic infections can cause a coated tongue, and sometimes a white tongue can be a sign of nutritional deficiencies or digestive issues.
FAQ 14: How do tongue piercings relate to a coated tongue?
Tongue piercings can directly cause or worsen a coated tongue. A coating often appears on newly pierced tongues — this is a completely normal bodily reaction and usually disappears within two to three weeks. However, tongue piercings can become infected due to the amount of bacteria in the mouth, and a coated tongue can then be a symptom of that tongue infection. Rankability Anyone with a tongue piercing should maintain strict oral hygiene and monitor the piercing closely for signs of infection during the healing period.
FAQ 15: Can a coated tongue affect your sense of taste?
Yes, quite significantly. Coating can cover taste buds and impair taste perception, with affected individuals commonly experiencing a reduced taste sensation. Internetmarketingninjas The film acts as a physical barrier between the taste receptors and food, causing flavors to seem muted, metallic, or bitter. Most people notice a clear improvement in taste sensitivity once the tongue coating is treated and the surface is cleaned consistently.
FAQ 16: What vitamin deficiency can cause a coated tongue?
Several nutritional deficiencies are linked to tongue coating and changes. Vitamin B12 deficiency is among the most commonly identified — in cases of coated tongue during menopause, quite often a vitamin B12 deficiency is the underlying cause. Colgate Iron deficiency can cause the tongue to appear pale and smooth rather than pink, and zinc deficiency has also been associated with white tongue in some individuals. A simple blood panel from your doctor can identify whether a nutritional deficiency is contributing to your symptoms.
FAQ 17: When should I see a doctor for a coated tongue?
You should see a doctor or dentist if the coating has lasted more than two to three weeks despite consistent oral hygiene, if the coating is unusually thick or heavily discolored, or if it is accompanied by pain. You should consult your dentist about a white tongue if it is painful, the coating lasts for longer than three weeks, or you are concerned about changes to your tongue associated with the coating. Quora White patches that cannot be scraped off, difficulty swallowing, or a burning sensation are additional red flags that require immediate professional attention.
FAQ 18: Can children develop a coated tongue?
Yes, children of all ages can develop a coated tongue. In newborns and infants, oral thrush caused by Candida is a particularly frequent cause. Parents sometimes confuse it with residual milk, but unlike milk residue, thrush patches do not wipe away cleanly. White tongue is usually harmless and temporary Sarah Worboyes in children, and in older children the causes mirror those in adults — inconsistent brushing, mouth breathing, dehydration, or post-antibiotic changes. Teaching children to include tongue cleaning in their brushing routine from an early age is an excellent long-term preventive habit.
FAQ 19: Does drinking more water help with a coated tongue?
Yes, hydration is one of the simplest and most effective interventions. Saliva is the mouth’s natural cleaning agent, and when water intake is insufficient, saliva production drops and bacterial buildup accelerates. Most people can get rid of white tongue by practicing good oral hygiene and drinking plenty of fluids to prevent dehydration. Drinking at least eight glasses of water daily is recommended as a starting point. Sarah Worboyes Staying hydrated throughout the day — rather than drinking in large amounts infrequently — provides the most consistent benefit for keeping the tongue clear.
FAQ 20: What is the difference between a coated tongue and leukoplakia?
This is a clinically important distinction. A coated tongue is a broad surface buildup of debris and bacteria that can usually be at least partially scraped away, and it typically clears with improved oral hygiene. Leukoplakia refers to thick white patches that are firmly attached to the tongue or mouth lining, cannot be scraped off, and do not resolve with hygiene changes alone. The white patches associated with leukoplakia can eventually progress to oral cancer Sarah Worboyes, which is why they require professional evaluation and monitoring. Any white patch that persists and cannot be removed by scraping should be assessed by a dentist promptly.